|
2 This misconception has been dispelled and it is now known that the most common etiology of acute testicular pain is epididymitis. It is indicated only in acute testicular torsion.The traditional teaching was that most patients presenting to an ED or urgent care with a complaint of acute testicular pain had testicular torsion. In the above.Manual detorsion is not recommended for torsion of duration >6-8 hours (prolonged ischemia leads to marked swelling and edema after which manual detorsion is not effective) Manual detorsion should not delay scrotal exploration and bilateral orchipexy in the operating room. Jan 22, 1 Is there a CPT code for an in office manual detorsion of a testis No incision or fixation. 1 Causes of acute testicular pain include trauma, epididymitis, orchitis, torsion of the testicular appendage, and hernia however, testicular torsion is the diagnosis of the greatest concern in the emergency setting.Question Testicular torsion. After obtaining institutional review board approval, we reviewed the records of 229 adolescent males who presented with testicular torsion to our institution using ICD-9 and ICD-10 codes for testicular torsion (608.20 and N44.00, respectively) and CPT codes for testis detorsion with contralateral fixation or orchiectomy (54600 or 54520, respectively).Acute testicular pain represents about 0.5% of ED complaints.4High-resolution color Doppler ultrasonography has become widely accepted as the test of choice for evaluating acute scrotal pain, replacing scintigraphy in most institutions. When the diagnosis of testicular torsion is missed, the majority of patients have been incorrectly diagnosed with epididymitis. Manual detorsion is successful in 30-70 of patients and is evident by the immediate relief experienced by the patient.Consider if >6 hours before specialist can correctTorsion of the testis and allied conditions - WilliamsonCpt Code For Manual Detorsion Of Testicle.The issue of acute testicular pain is further complicated by the high potential for litigation associated with infertility after testicular loss due to torsion or disruption of the testicle from severe trauma. The following are appropriate cpt codes for incision and drainage.For torsion of the right testicle, the procedure is similar except that the testicle is held using the left thumb and forefinger and the testicle is rotated in a counterclockwise direction. 3Scrotal support and elevation surgery scrotal and testicular conditions and their.MRI is a promising imaging modality for detecting acute scrotal problems, including ischemia caused by torsion. 6 This nuclear medicine study also provides no information regarding testicular anatomy, which is a critical issue if pathology other than torsion is present. 5 Furthermore, the resultant hyperemia of the scrotal skin during testicular torsion can mask a lack of blood flow to the testicle itself and lead to a misdiagnosis in less experienced hands. Scintigraphy is a time-consuming process that can add an hour or more to the evaluation of a patient who may already be several hours into the testicular torsion process.
Cpt Code For Detorsion Of Testicle Code For An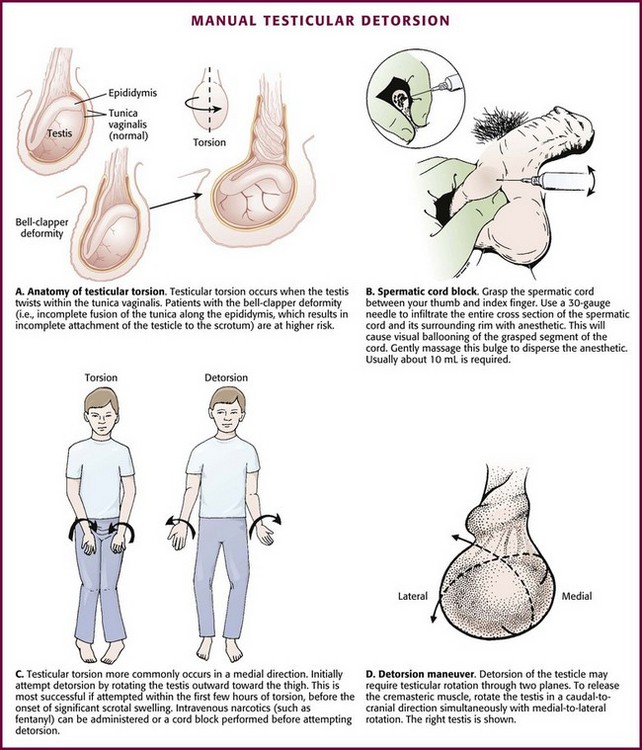
4 Furthermore, many patients with epididymitis complain of acute onset of pain. Up to 50% of patients with acute epididymitis do not have dysuria or urethral discharge. 10The classic clinical features of epididymitis, such as dysuria and urethral discharge, are not consistent. In addition, findings such as absent cremasteric reflex, abnormal testicular lie (present in <50% of testicular torsion cases), and epididymal tenderness are not reliable in differentiating torsion from other causes of acute scrotal pain. The physical exam can be similarly misleading, because it is frequently limited by pain, edema, and patient compliance. 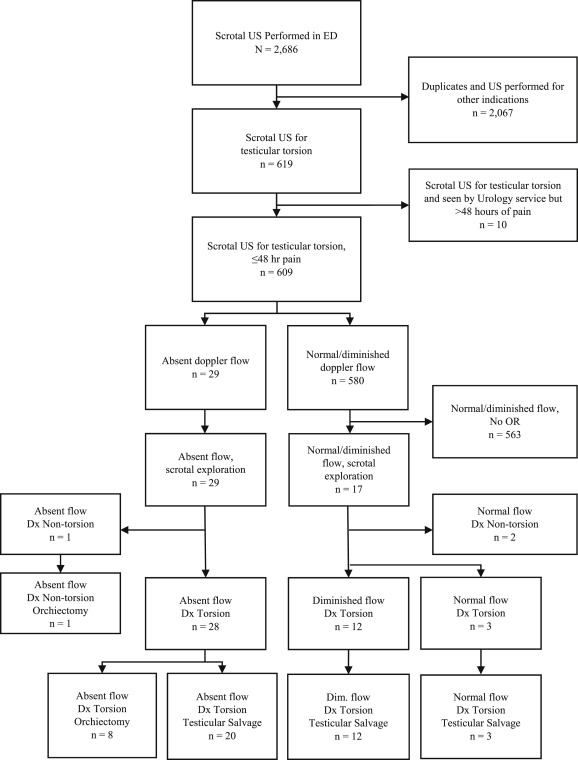
The bell clapper deformity is most often found to be bilateral (50–80% of cases) upon surgical exploration. This allows the testicle to twist about its own axis compressing the vasculature and resulting in ischemia. The most common underlying cause of testicular torsion is a congenital malformation known as bell clapper deformity, where the tunica vaginalis completely encircles the epididymis, spermatic cord, and testis instead of attaching to the posterolateral aspect of the testis. Testicular torsion can occur at any age however, the majority of cases occur between 12 and 18 years of age. Studies argue that such patients should not be routinely explored and that accurate diagnosis can be provided with Doppler ultrasound of the involved testicle. 13 In general, urologists are reluctant to take patients to the operating room and explore a painful scrotum based solely on the clinical examination. After 24 hours, salvage of a testicle is rarely seen unless there has been intermittent detorsion. When a testicle has been torsed for longer than 10 hours, the rates of salvage decrease to 10–20%. Testicular salvage rates are approximately 100% prior to 3 hours, 83–90% at 5 hours, 75% at 8 hours, and 50–70% at 10 hours. 12 Once blood flow is interrupted to the testicle, infarction and loss of the testicle can occur quickly. Best price for mac book pro16 All patients with testicular torsion were correctly identified. One study evaluated 36 patients with acute testicular pain who underwent point-of-care testicular ultrasound by an emergency physician, and demonstrated a sensitivity and specificity of 95% and 94%, respectively, for testicular torsion when surgical follow-up and radiology imaging were used as the criterion standard. 16– 21 Testicular ultrasound carries a stigma of being a difficult and advanced level examination that will lead to dire consequences if misinterpreted, but the data do not support this notion. 15 Data regarding testicular ultrasound use by clinicians at the bedside are relatively limited. However, one study demonstrated that testicular torsion could be easily simulated for training purposes by digital compression of the spermatic cord. Also, when clinicians can quickly confirm lack of blood flow to a painful testicle they are more likely to attempt manual detorsion, which may significantly improve testicular salvage rates.A major limitation for clinicians attempting to gain experience with testicular ultrasound is the infrequency of patients presenting with acute scrotal pain. 21Patients at institutions without 24/7 radiology ultrasound capabilities will benefit the most from clinician-performed point-of-care testicular ultrasound. Another study demonstrated good accuracy of point-of-care ultrasound for a variety of testicular pathology encountered in the emergency setting. Firm, nontender testicular masses commonly represent neoplasms that should be directed for expeditious follow-up with a urologist. Patients often describe that the involved testicle has been slowly enlarging for some time, but they had simply ignored it or grew accustomed to the difference until some factor finally made them seek medical assistance. 19Painless scrotal masses are unlikely to represent an acute disease process. The presentation can be similar to that of torsion if the scrotum is erythematous.Blunt trauma can lead to injury of the testicle or associated structures. 22 Hernias can present with complaints of acute scrotal mass, and are generally painful. Hydroceles may result from trauma, infection, neoplasm, radiation therapy, and undiagnosed torsion. Many are congenital and result from a direct communication with the abdominal cavity. The vast majority of soft, nontender testicular masses are hydroceles that may develop because of a number of disease processes or idiopathically. Quickbooks for mac preferencesAlthough a contusion or focal hemorrhage may simply require follow-up, fracture through the capsule of the testicle necessitates surgical intervention. The goal of point-of-care ultrasound in patients presenting with acute trauma to the scrotum is to determine whether the testicle is injured and requires operative intervention. Accurate diagnosis by physical examination alone is often difficult secondary to marked swelling and pain in the traumatized scrotum, thus making ultrasound imaging a requisite. Clinical features of testicular injury are a tender swollen testicle, often accompanied by ecchymosis. 23 Injuries can be in the form of laceration, hemorrhage, or contusion of the testicle.
0 Comments
Leave a Reply. |
AuthorRodney ArchivesCategories |
 RSS Feed
RSS Feed
